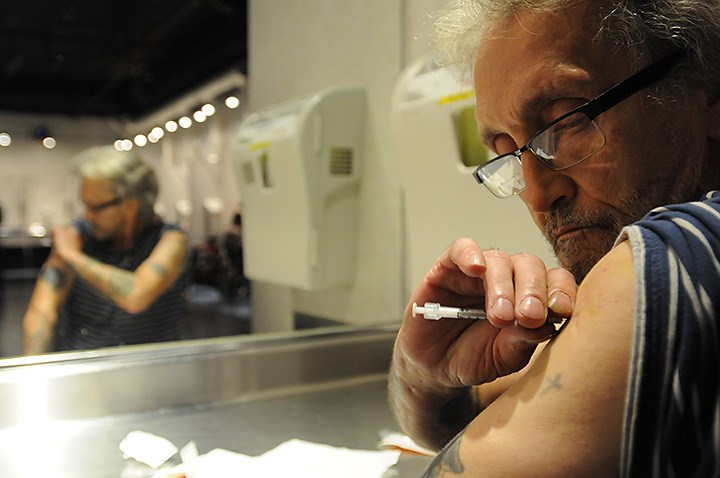
The procedure is hard to watch: A 52-year-old woman takes a syringe filled with heroin and carefully inserts it into a vein in the side of her neck.
As she pulls out the syringe, she checks herself in the mirror and notices a trickle of blood coming from the tiny wound. She wipes it with a sterile pad and she’s done.
Gail Hunt is high.
She will complete the same procedure at least twice more on this day. And she will do it in the Insite supervised injection site, where she’s been a client for nine years.
“It’s safe and if anything happens to me, there’s trained professionals here who can help,” she said, sitting in an injection booth last Thursday at the facility on East Hastings.“I’ve watched people go down in front of me — overdose — and the staff are there right away. We haven’t lost one person in here.”
Hunt, who began using heroin to mask the pain from breast cancer, is a regular at Insite, which marks its 10th anniversary of operation this month. The facility’s longevity is a remarkable feat considering it originally opened Sept. 21, 2003 as a three-year scientific experiment. Ten years later, and after more than two million injections without an overdose death, Insite continues to be the only legal site of its kind in North America.
But keeping the facility’s doors open has been a battle.
Prime Minister Stephen Harper and his government want Insite closed and fought unsuccessfully in the courts to shut down the service.
Despite a Supreme Court of Canada ruling in 2011 to allow Insite to operate indefinitely, the Harper government tabled a bill in June aimed at making it difficult for Insite to renew its licence in 2014.
The bill, called the Respect for Communities Act and supported by the Canadian Police Association, sets out a long list of criteria that critics say also dissuades other cities from applying for an exemption under the country’s drug laws to open an injection site.
The federal government’s campaign against Insite and advocates of injection sites comes despite a series of peer-reviewed studies showing the facility is doing some good for people.
Studies published in various medical journals including the Lancet and the New England Journal of Medicine concluded Insite saves lives and health care dollars, reduces disease transmission and does not increase crime or perpetuate active drug use.
Additionally, a recent Vancouver Coastal Health report revealed Downtown Eastside residents, a portion of whom are addicts, are living longer — from a life expectancy of 69.4 years in 1996 to 79.9 in 2012.
For 62-year-old drug user Larry Love, who also visited Insite last Thursday to inject himself with heroin, the alternative to a supervised injection site is not something he wants to think about.He remembers the mid-1990s when upwards of 200 people per year died of drug overdoses in Vancouver. If Insite closed, he said, the city would “look like hell again.”
“I just couldn’t imagine if this place wasn’t open, I just couldn’t imagine it,” said Love, overlooking the facility’s injection booths busy with people getting their next fix.
• • • • •
More than 1,200 people died of a drug overdose death in Vancouver between 1992 and 2000.
That’s an average of 150 fatalities per year.
In the past decade, that rate plummeted to 589 overdose deaths in the city, according to statistics supplied to the Courier from the B.C. Coroners Service. The 589 deaths occurred between Jan. 1, 2003 — nine months before Insite opened — and Sept. 3, 2013.That statistic could drop even more if the coroners service is unable to conclusively say the 69 deaths in 2012 and 43 to date this year were caused by drugs; many are still under investigation.
Regardless of the downward trend in deaths, no one in the medical or research community suggests Insite is the sole reason for the 50 per cent decrease. But a 2011 study published in the Lancet showed fatal overdoses within 500 metres of Insite decreased by 35 per cent after the facility opened. That 35 per cent drop compared to a nine per cent decrease in the rest of Vancouver.
Reaching a definitive conclusion on the reason for the drop in overdose deaths is difficult to measure.But it’s a fact the city has become more friendly to the drug user since the 1990s. More needle exchanges, treatment programs and drug outreach services exist in Vancouver. More heroin users are on the methadone program and some are participants in drug trials, which offer prescription substitutes in place of heroin. Vancouver has a drug court and a community court, whose mandates are aimed at getting drug-dependent criminals treatment and housing instead of sending them to jail.
And there’s been a lot of valuable research.
A study released in June from the Urban Health Research Initiative of the B.C. Centre for Excellence in HIV/AIDS tracked drug use patterns over 15 years in Vancouver.
The authors, which included scientists from the University of B.C.’s Division of AIDS, discovered a dramatic decrease in injection cocaine use and syringe sharing since the mid-1990s.
People suffering from infectious diseases are receiving better treatment and another report released last week by the B.C. Centre showed 29 injection drug users in the province were diagnosed with HIV/AIDS in 2012 compared to more than 400 per year prior to 1996.
When asked what role Insite played in the remarkable drop in HIV/AIDS cases, Dr. Julio Montaner, director of the B.C. Centre, pointed to a progressive province-wide strategy to stop the spread of the deadly virus, including access to free antiretroviral therapy drugs that can reduce HIV transmission.
That strategy, he said, coupled with the services of Insite and its detox facilities — called Onsite and spread over two floors above the injection room —play a big part in preventing drug users from contracting HIV/AIDS.
Insite, which has more than 12,000 registered users, is stocked with clean injection equipment and staffed with nurses and counselors that educate clients about safe injection practices.
At Onsite, doctors, nurses, mental health workers and counselors work together to help stabilize recently sober users and plan their next steps in life.
“Why are we the only jurisdiction in the world that is seeing dramatic decreases in HIV cases all together, but more so in the intravenous injection use?” Montaner said, then answered his own question by again pointing to “low-threshold” services such as Insite which serves street-entrenched drug users prone to infectious disease.
• • • • •
In 2012, a total of 488 people completed Onsite’s treatment program. Insite counsellors also made more than 5,000 referrals to other social and health service agencies, the majority of which were for detox and addiction treatment.
Onsite’s first floor has 12 beds for clients to detox and the second has 18 beds for people such as Robert Mayzes, a longtime drug user who is six weeks sober.
Mayzes, 57, spent one week in detox and the past five weeks getting himself healthy and focused to move into housing. He was recently diagnosed with terminal cancer. He is candid about his reason to get sober. “I want to die straight — it’s that simple,” he said, sitting on his bed in a small room at the back of the building. “With the time I got left, I want to live like normal folks."
Without Insite and the staff that has helped him, Mayzes said, he would have probably done “the big fix” — meaning taking enough drugs to kill himself. He spends his days creating art and writing down some of his life experiences. He used to deal drugs, was a thief and a robber. He’s been stabbed twice, thrown off a three-storey parkade and still has shrapnel is his right knee from a shooting in the Columbia hotel.
Mayzes’s decision to get sober has not only been good for him, he said, but he was surprised at the reaction from other drug users. “Two people I know came in here and said they were in here because they saw me doing this. They’re looking at me and saying, ‘Rob, if you can do it, I can do it.’ Being an example like that is amazing.”
• • • • •
At a café down the street from Insite, Donovan Mahoney is talking about his road to recovery.
A long-time client at Insite, Mahoney agreed to seek treatment for his heroin addiction.
The 37-year-old chronic offender said Insite staff got him into Onsite and treatment centres in Vancouver, New Westminster and Mission.
It’s been a struggle, said the former construction worker, having relapsed a few times. But by the end of September, he will have been sober for 18 months.
When we met for an interview last Thursday, Mahoney was dressed in a trendy black hoodie, shorts and carrying a backpack with a yoga mat. He had just come from a yoga class in Kitsilano. Mahoney is now a yoga instructor, teaches out of his apartment and has a strong interest in photography. He’s working on a photo exhibit, mainly of images from the Downtown Eastside, for a show at the Interurban gallery in March. He is on Facebook and has active Twitter and Instagram accounts, which he uses to tell his story and show his photographs.
His story is a sad one: His dad died from a fall down a staircase on a Christmas Eve when Mahoney was six. His mother killed herself a year later. His parents had severe addiction issues. Mahoney was adopted at 7, eventually got hooked on drugs and embarked on a life of crime that he says totals 160 convictions.
His drug use hit an all-time low in 2006, when he went into a coma for 17 days after an overdose. He shows a tattoo on his left forearm that has the dates — Dec. 4 to 21 — etched in his skin, next to the words, “a gift of love.”
"I remember thinking that’s a good note to stop using on. That moment was kind of like, yeah I’m done. I never wanted to get loaded again.”
But he did, leading to a suicide attempt last February.
He climbed scaffolding outside the Regent hotel and planned to do enough drugs so he would pass out and fall to his death. That act was captured on a television series called The Beat, which features Vancouver police officers working in the Downtown Eastside.
He later got picked up for shoplifting, went back to jail and then contacted Insite staff again to get him into treatment. He has this to say about Insite.
“In one sentence, it’s kept me alive long enough to start living.”
For those critics of Insite, Mahoney wants them to consider how much money his sobriety is saving taxpayers. Think about the policing, ambulance, hospital and court costs associated to a drug-addicted criminal, he said.
Never mind, he continued, the cost of treating someone with HIV/AIDS or other infectious diseases such as Hepatitis C, which he has neither.
Or, there’s this: The sight of him overdosing in Yaletown in front of a young family — which he did — and the scar an incident like that leaves on the community.
“That’s traumatizing for everybody,” he said, estimating his sobriety saves taxpayers more than $150,000 per year.
• • • • •
It costs $3 million per year to operate Insite, which is run by Vancouver Coastal Health in conjunction with the PHS Community Services Society.
It’s money well spent, said Dr. Patricia Daly, the health agency’s chief medical health officer, who pointed out Insite’s budget is a small percentage of the agency’s annual $44 million addictions budget, which is devoted largely to treatment and drug prevention programs.
Daly said she wants more injection sites to open in Vancouver but integrated within health clinics. She’s convinced of Insite’s benefits.
“In my view, it would be great if there wasn’t another article about this in 10 years — that it was just an accepted public health practice and we’ve moved on to other things,” she said.
Tom Stamatakis, president of the Vancouver Police Union and Canadian Police Association, is one of those people Daly will have to convince before injection sites are an accepted health practice.
Stamatakis has always questioned the effectiveness of Insite and agreed to be quoted in the Harper government’s press release in June announcing the introduction of the bill aimed at stifling any further applications for injection sites.
“While treating drug addiction is an important goal, my experience in Vancouver is that these sites also lead to an increase in criminal behaviour and disorder in the surrounding community and have a significant impact on police resources, and that’s why it will be vital for the views of local police to be taken into account,” he said in the release.
He elaborated on his views in an interview with the Courier, saying he continues to see rampant injection drug use outside his office in the Downtown Eastside. He pointed out the drugs people are using at Insite are purchased illegally on the street from dealers working in front of businesses and residences. He prefers money be spent on treatment, prevention and education around drug use.
“Are we encouraging people to make better choices? Are we treating people and getting them into better lifestyles — getting them away from drug use?” he said. “I don’t see it, I don’t see those significant gains.”
Stamatakis said he read the studies from the B.C. Centre for Excellence in HIV/AIDS and others and has always tried to keep an open mind about how best to tackle the city’s drug problem.
But, he believes, the studies are done largely by proponents of injection sites who are relying on data from users.
He questioned the objectivity of the studies.
“Anybody in the medical profession or policing or anywhere who dares to say anything that’s less than supportive, you’re widely criticized and they attack your credibility and accuse you of all kinds of terrible things,” said Stamatakis, anticipating pushback for his comments.
His views are in contrast to those of the premier, the mayor and the police chief, who are all on record of supporting Insite.Their support should factor favourably for Insite getting its licence renewed in March 2014.
In the meantime, the Harper government continues to discount the studies and the demands for more injection sites in Canada.
And that attitude is what enrages Montaner, who is considered to be one of the world’s leading HIV/AIDS doctors. The Harper government, he said, has “gotten away with murder.”
“The draconian, Machiavellian manoeuvres emerging from Stephen Harper’s office have been able to prevent implementation of these types of programs across the country at the cost of many lives that, ultimately, they are responsible for.”
[email protected]
t
twitter.com/Howellings