For more than three years now I’ve been depending on virtual doctors in British Columbia for care after not being able to find a family doctor.
It seemed like I had tried everything: I phoned doctors, went to walk-in clinics, applied online for a family doctor and even used the province's online wait-list directory to try and secure one. I’d be remiss if I didn’t add that I am a healthy person with no major health concerns and can navigate the online world easily.
After getting COVID-19, having an injured foot, needing prescriptions, and trying to find an allergy specialist, I turned online each time and the process was not only seamless but effective.
I tested positive for COVID-19 back in December. Thankfully, my experience with the virus was resolved in a few days and I only lost my sense of smell for a few months afterwards. I have received three doses of the vaccine and navigated getting COVID-19 without a family doctor, which I believe is the case for many British Columbians.
During my time living and working in Victoria, also described by some as the Garden City, my allergies were sent into full swing.
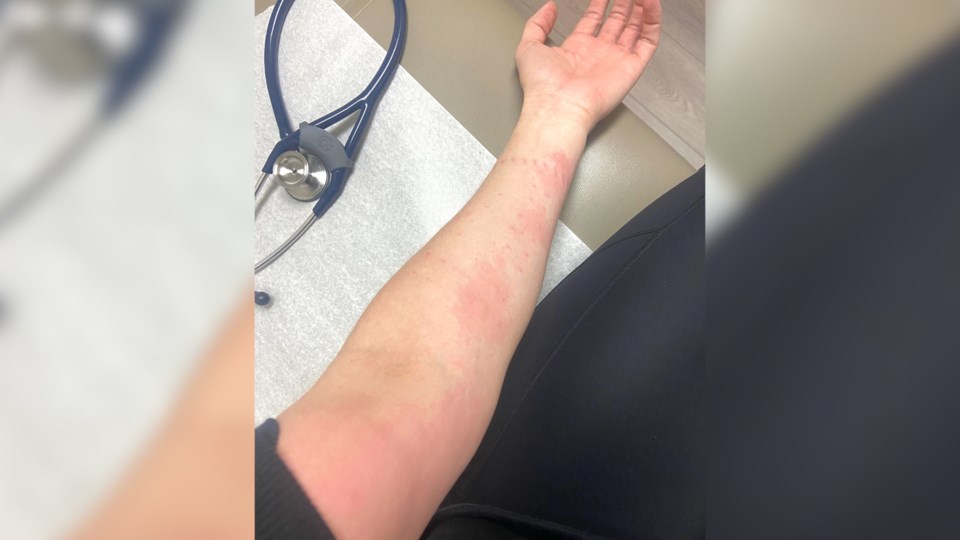
I desperately needed to get them under control. As soon as I stepped outside, I'd have sneezing fits, itchy eyes and a sore throat. Not a great combination during the pandemic.
I’d never experienced severe allergies during my time in Ontario, Kelowna or Whistler. So without a family doctor, I searched the internet for an online one who could help. I was able to quickly schedule a virtual appointment and was given a prescription for a nasal spray, eye drops and an antihistamine. The prescription was forwarded to my nearest pharmacy and I picked it up that day.
After a few months, I followed up with a different virtual doctor, hoping to get some more relief as the medicine was not doing the trick. I was referred to a specialist and put on a year — yes, a one-year wait-list — to see an allergist in Victoria.
I’ll never forget receiving that text message for my appointment and frantically calling them thinking I missed the appointment, only to be promptly told that it was actually for the following year.
Between that text message and now, I've made the move to Vancouver. Turns out I am allergic to almost every tree in Vancouver, and cats.
In November, I will return to Vancouver Island and start immunotherapy for my allergies.
As I began settling into my new Vancouver home, I fully accepted that getting an online doctor would be just as hard as it was on Vancouver Island.
To my surprise, I received an email in May stating that my name had been drawn from a pool of applicants. (I had added my name to B.C.'s Health Connect Registry a couple of years back.)
"We are happy to accept you as a patient if you are still looking for a primary care provider. You can reach us by phone,” read the email.
I hit the jackpot, medically speaking.
There was just one problem: I didn’t live on the Island anymore. And unfortunately, they only accept patients who reside there.
Since moving to Vancouver, I’ve used a virtual doctor for prescriptions and even for help with an injured foot.
I was able to secure a virtual appointment and have them look at my foot over video. They suggested I see a physiotherapist. After a few weeks with no improvement, I scheduled a new appointment and was referred to get an X-ray and a podiatrist.
The very same day I walked three blocks from my home to the X-ray centre and had my foot screened with zero wait time. Thankfully, it wasn't broken.
Navigating the virtual doctor world has been efficient for me, but I am aware that I am technology-savvy and I have not had any major health complications.
The Vancouver Division of Family Practice has some ideas to find a primary care provider, including asking your friends and family members for recommendations.
Another recommendation is asking your walk-in clinic doctor if they'll accept you as a new patient. Better yet, find clinics that are publicly advertising that they're accepting new patients.
Today, I'm back to square one, trying to find a doctor.
If you know anyone, please shoot me an email: [email protected].
A longitudinal relationship with a doctor is key
A Vancouver-based family doctor and assistant professor in the Department of Family Practice at the University of British Columbia says virtual doctors and virtual care is an effective way to provide care but a family doctor provides longitudinal care.
Rita McCracken says virtual doctors were one of the few silver linings of the pandemic.
"Virtual technology, the telephone, Zoom or any other virtual platforms are really an essential element that we have seen be used really effectively in primary care,” she says.
She's cautious about virtual technologies and virtual walk-in clinics as the research shows it misses the mark in one important way.
“Primary care improves the health of a population, decreases mortality, so people actually live longer with access to primary care, and we reduce costs to a system overall, that is predicated on a longitudinal relationship, not a one-off virtual visit with a stranger,” she says.
Having an episodic relationship with a new person virtually does not offer the same care, she adds.
“We really want to be maximizing that longitudinal relationship; whether or not that happens in person, or virtual, we don't really have any good research about that,” says McCracken.
Can virtual doctors work for remote communities?
Virtual doctors can be successful for remote communities but come with challenges.
For McCracken, she started using video sessions but found her clients preferred the telephone.
“In Canada, almost everybody has access to the telephone. And that works really well.”
Virtual walk-in clinics require people to create an account and use a specialized platform. McCracken says that might not always be possible for the elderly or some people who don’t have internet access in remote areas.
"You might need to have a certain bandwidth available... a certain speed of internet.”
McCracken says it would be better if there was an office or clinic for virtual doctors.
"It would be better if we could create a work environment where those doctors who are working virtually were able to work in a place where they could create a relationship and provide longitudinal community-based care," she says.
McCracken believes the “quick fixes” of an online virtual walk-in clinic are a placeholder for now.
“It's not going to take the place of the real change that needs to happen,” she says. “Having a longitudinal relationship with a family doctor is the thing that is going to help the health of Canadians and we need to figure out solutions to make that happen.”




