 colinross1 Colin Ross, 37, continues to battle a heroin addiction while pushing back against stereotypes associated to drug users, the homeless and people living with mental illness. Photo Dan Toulgoet
colinross1 Colin Ross, 37, continues to battle a heroin addiction while pushing back against stereotypes associated to drug users, the homeless and people living with mental illness. Photo Dan Toulgoet
Being Colin Ross can be complicated.
His 37-year-old life, as far back as he can remember, has been this way.
Why?
It’s a long story.
But to tell it, the former chef wants you to reconsider the first impression you may have of him after studying his photograph: yes, he’s a heroin user, looks a little rough and is one of those determined guys who roots through dumpsters for discarded goods that he turns into a profit on the street.
Sit him down in a Main Street café, with a coffee in front of him, and the Edmonton-born, Canmore-raised “hurtin’ Albertan” will tell you there’s more to his life than a dependency on drugs and the grind of binning and vending.
Ross lives in a subsidized apartment in the West End, where he creates art with some of his dumpster finds. He remains connected with his sister in Kerrisdale and regularly visits his niece and baseball-playing nephew.
Then there’s his long-held passion — educating students, doctors, politicians and others interested in his life as a drug addict. He estimates he’s done at least 60 talks in eight years at schools and conferences.
The sharing of his story was inspired by his membership with the Mayor’s Task Force on Mental Health and Addictions, the city’s advisory committee of people with lived experience and his participation in the Mental Health Commission of Canada’s At Home/Chez Soi housing experiment and speakers’ program.
In April, he spoke to city council on behalf of Megaphone Magazine to help secure an $85,000 grant to set up a speakers’ bureau. The goal is to continue the work of the At Home program, his work with the city and focus on removing the stigma many in the public attach to drug users, the homeless and the mentally ill.
“I’m very passionate about changing the way people look at people who are struggling,” he said in one of a series of interviews with the Courier in recent months. “I’m a decent person and a drug user. It doesn’t have to be two different things.”
Trust him, he said, he didn’t choose to lead the life of a drug addict. That reality can be traced to an untreated bipolar disorder, severe anxiety and having alcoholic parents who separated before his first birthday.
Depression, anger, isolation and going through his own bout of alcoholism have been other experiences. Ross, who had a criminal record as a juvenile in Alberta — mainly for petty stuff such as shoplifting and vandalism — has lived on the streets and overdosed once.
He himself is amazed he's still lucid, still here.
The frequent illicit drug death reports from the BC Coroners Service suggest Ross is vulnerable: the largest group of people dying from drug overdoses are white men in their 30s, who have had a long history of addiction.
So much of the reporting about the opioid crisis has focused on the dead.
Ross is a survivor.
How has he done it?
The answer involves a caring sister, a good doctor, finding his own apartment, trying a variety of treatment options, being asked to share his story with people in power, some luck and an internal drive to stay alive.
That drive, as well as some of the frustrations of managing an addiction, was evident on the days the Courier accompanied Ross to a pharmacy, a doctor's appointment, on walks through the Downtown Eastside and visits to coffee shops.
What follows is a chronology of sorts, beginning in April and finishing in July, that provides a glimpse into the life of a man who doesn't know that he'll ever be drug-free, but is determined to get stable and be more present in the lives of others.
‘Warm hug from God’
In the back room of Pier Health Resource Centre, near Main and Hastings, Ross is sitting in a chair as nurse Amanda Pelcz prepares a dose of liquid hydromorphone, a pain management opioid designed to reduce cravings for heroin.
It's a mid-morning on a Thursday in late April. The sun is out and Ross’s bike ride from his West End apartment has left him wiping his brow with paper towel.
Ross is one of 53 participants in the pharmacy's injectable hydromorphone program. He became a patient in June 2017. Twice a day, he injects himself under the supervision of a nurse. Then he takes an oral dose of hydromorphone in the evening at his neighbourhood Shoppers Drug Mart.
It’s a daily routine that he admits can be onerous, but has substantially decreased his dependence on heroin. It’s also meant he doesn’t have to spend as much time binning to pay for his heroin habit, which at its high point can reach $40 a day.
“When you see people beat to shit, it’s because of what you’ve got to do to get the drugs,” he said. "Coming in here, I deal with a pharmacist and a nurse as opposed to some dealer in a piss-smelling back alley. It’s a completely different atmosphere, which puts you in a different head space. It gives you some dignity, is the other thing.”
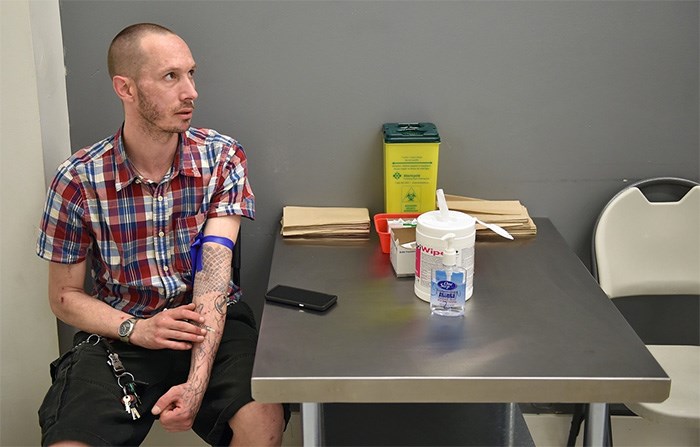 Colin Ross at the Pier Health Resource Centre near Main and Hastings, preparing to inject liquid hydromorphone into his arm. Photo Dan Toulgoet
Colin Ross at the Pier Health Resource Centre near Main and Hastings, preparing to inject liquid hydromorphone into his arm. Photo Dan Toulgoet
Ross takes the syringe from Pelcz and injects 50 milligrams of hydromorphone into his tattooed left arm. He gives the drug a few moments to take effect before he explains the sensation.
“There’s a little initial rush, which I like to call a warm hug from God,” he said. “It’s like a deep breath. All your muscles — everything — is relaxed. It’s like a sigh, a full body sigh.”
But it’s not heroin, which he developed an addiction to as a teenager.
“Good heroin would do the same thing in a lot ways, but do it way better. Like decaf to real coffee.”
Over the years, Ross has tried methadone, Suboxone and a steady oral dose of hydromorphone, which doesn’t produce the euphoria experienced with injection.
None, he said, has been as effective as heroin in treating his mental and physical pain; he has arthritis in most of his joints and various other nagging injuries.
Ideally, he wants to try diacetylmorphine, which is medical grade heroin. The Crosstown Clinic, located a few blocks from the pharmacy, is the only clinic in North America that offers the drug to chronic drug users.
Ross has expressed a desire to his doctor, David Tu, to become a patient. But the popularity of the program, which has seen impressive results where patients have stabilized enough to secure housing and jobs, has meant a long waiting list.
Tu is the reason Ross is more stable than he’s ever been. It is difficult for Ross to talk about his doctor without getting emotional. On the advice of a friend, he searched out Tu more than seven years ago, who took him on as a patient.
“He’s a saint, he saved my life,” Ross said after taking the required 15 minutes in the pharmacy’s waiting room to relax and ensure he’s showing no ill effects from the hydromorphone. “He’s a wonderful doctor, just a good human being. He really understands addiction. He’s done a lot of good for a lot of people.”
‘Therapy is a bridge’
It was Tu who got Ross into the pharmacy’s injectable hydromorphone program, which was developed by colleague, Dr. Christy Sutherland, the medical director of the PHS Community Services Society.
Sutherland entered into a partnership with Pier owner, Bobby Milroy, to set up the innovative and ground-breaking service, which provides another treatment option for those unable or not interested in accessing the Crosstown Clinic.
“You end up helping a group of people who would not otherwise be allowed to be helped,” said Milroy, standing outside the pharmacy on the day of Ross’s visit in late April. “As a result, you’re saving lives. It doesn’t work for everyone, and I don’t think it will be everyone’s choice of treatment, but it’s simply one more option.”
Ross was Tu’s first patient to participate in the pharmacy’s program.
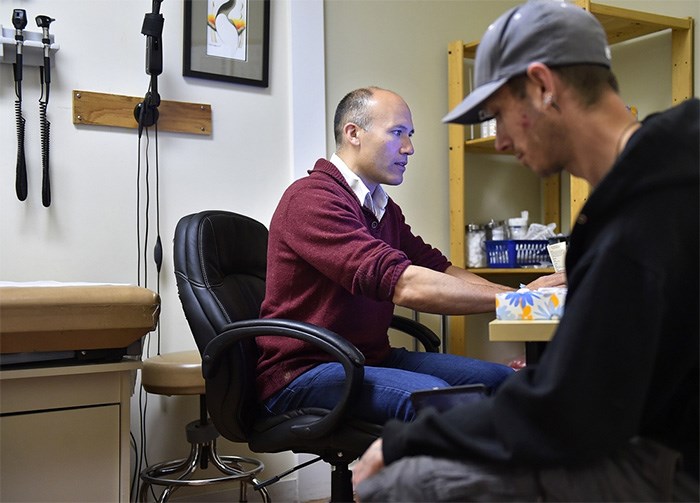 Dr. David Tu meeting in his office with Colin Ross. Photo Dan Toulgoet
Dr. David Tu meeting in his office with Colin Ross. Photo Dan Toulgoet
Over lunch at a restaurant adjacent to his office at the Vancouver Native Health Society on East Hastings, where he sees about 70 patients on drug replacement therapy, Tu explained the referral.
He reiterated what Ross said about methadone, Suboxone and oral hydromorphone not providing the results they both hoped for.
“None of that allowed him to not continue to use injectable street opiates,” Tu said. “And when you’re injecting on top of what’s being prescribed to you, you’re going to develop a higher tolerance and experience those same withdrawal symptoms. So you’re not going to get that stabilizing.”
For some context to Ross's situation, Tu recounted a brief history of opiate replacement therapy in the United Kingdom, Switzerland and other parts of Europe, which have been progressive on drug policy and harm reduction initiatives for years.
But what the body of literature concluded in those countries' experiments, and holds true in North America, is that about 10 per cent of addicts will not stabilize by oral therapy alone.
Diacetlymorphine and injectable hydromorphone were found through various studies to be the only option for that 10 per cent.
Tu pointed to the North American Opiate Medication Initiative, more commonly known as the NAOMI trials, which revealed almost 10 years ago that study participants in Vancouver could not accurately discern the difference between the effects of diacetylmorphine and injectable hydromorphone.
Hence the reason to get Ross started on the injectable hydromorphone program.
“There’s going to be five to 10 of my patients at one time that are not successfully stabilizing on oral for whom you’ve got to look for something else,” Tu said. “It doesn’t make sense to keep on trying something that’s not working.”
Tu said Ross experienced a “dramatic turn” in the first four months of his therapy and found the hydromorphone helped him stabilize and focus on his work in the harm reduction community.
The goal was to free Ross, whose monthly welfare cheques help pay for his rent, food and phone bill, from the stress of binning and vending, effectively decreasing his use of heroin.
“He’s starting to see himself as a good person, someone who can contribute,” he said. “And when he has that, it will drive him to make choices that will likely be more positive and affirming, and put him on a good path.”
Tu continued:
“The therapy is a bridge — hopefully — to some sort of transformation. It can be a very long bridge, it could be a shorter bridge. But it’s a means to an end, as opposed to an end itself.”
‘You’re always playing Russian roulette’
The path of that bridge took a turn two weeks after the Courier’s interview with Tu.
Ross was no longer participating in the injectable hydromorphone program. The hydromorphone was “making me feel really gross, which is really weird because I’ve always liked it.”
The routine of having to bus or bike to the pharmacy twice a day was also grinding him down. He had been doing this for almost a year, living a life where he was tied to the pharmacy.
That’s what he told Tu during an appointment in mid-June. A few weeks prior, Tu prescribed long-acting morphine capsules for Ross, which cut back his visit to a pharmacy to once a day.
Tu to Ross: “How do you feel about continuing on the long-acting morphine?”
Ross, sitting in Tu’s office: “It’s not ideal, but I wouldn’t say it’s upsetting me or anything like that.”
The conversation shifted to talk about the Crosstown Clinic and diacetylmorphine. Ross agreed to visit the facility while Tu would again try to get him in the program.
Ross: “I’ve actually never been in there, but I think I know a lot of what goes on. I’ve never done diacetylmorphine, but I’m assuming it would be something I’d like more.”
In the meantime, Ross hoped to get a prescription from Tu for several doses of long-acting morphine that he could take with him on a week-long trip to northern Alberta. He was feeling stable enough to return to his home province to attend a music festival.
His father, who had remarried and had kids, would be there. So would a lot of friends. He needed to recharge, he said, and get out of the city for a while. He raised money through a GoFundMe campaign for a plane ticket; two relatives donated the money.
Tu agreed to write a prescription, but had more questions for Ross.
Tu: “How has your stress level and mood been over the last little while?”
Ross: “For the most part, pretty good. I’ve been a little stressed out and kind of pissed off a bit, but it’s been in the face of things that would really stress anybody out.”
Tu: “Yeah.”
Ross: “I haven’t been off the deep end. I haven’t had a day where I was really feeling uncontrollably angry just for being angry, or being set off and not being able to calm myself down.”
Tu: “So you’ve been able to maintain a kind of equilibrium?”
Ross: “Yeah.”
Tu: “More good days than bad days?”
Ross: “For the most part, it’s been pretty good to be honest.”
Tu reminds of him of the contaminated drug supply that killed 365 people in Vancouver last year, and has killed 165 in the first five months of this year. More than 1,400 people died across the province last year, with the majority of deaths linked to fentanyl.
Ross’s response to Tu, and one he repeated to the Courier several times, is that he’s careful when using drugs. He uses injection sites when there are no lineups and always uses a small amount of heroin for his first injection. He ensures he's around people equipped with the overdose-reversing medication, naloxone.
Even so, Ross overdosed about a year ago in an alley outside the Washington Hotel, near Main and Hastings. He regained consciousness in the hotel's injection room, before being transported by ambulance to St. Paul's Hospital.
“You’re always playing Russian roulette, but for me it’s as close to playing with a gun full of blanks," he said, describing his overdose as "minor" and believes to this day the naloxone wasn't necessary. "I never say I’m not taking any risks, but I’m as risk-free as you can possibly be.”
 Bir Kaur O’Flaherty, Colin Ross’s sister, became a guardian to her brother when he was 15. Photo Dan Toulgoet
Bir Kaur O’Flaherty, Colin Ross’s sister, became a guardian to her brother when he was 15. Photo Dan Toulgoet
Special bond with sister
His sister, Bir Kaur O’Flaherty, has heard him say that a lot — that he’s careful, not to worry, he’ll be fine.
It's little comfort for someone who pays attention to the news and hears story after story about the opioid crisis and how it's devastated families across the province.
"It only takes one time, and that's it," she said, sitting on a sofa in a cafe at the Jericho Village shopping centre. “But I have a practice and belief in my life that if he's going to die, he's going to die. I would, of course, be devastated, but it doesn't matter what I do to not make it happen, I just have to let it go."
The siblings have a special bond, with O’Flaherty taking responsibility for her brother when he was 15; she was 18 at the time, and recently moved from Alberta to Commercial Drive.
She has watched her brother get entrenched in a drug lifestyle, argued with him about it — which resulted in long stretches of not talking to each other — and tried to get him help.
A few years ago, she was successful in helping him get into Onsite, the detox centre above the Insite supervised injection site on East Hastings; Ross has been through various detox centres in B.C. and Alberta at least seven times.
She's listened to him, offered advice and has been like a mother to her brother.
Ross often jokingly refers to his sister as the “black sheep” of the family. She’s married, with two young children, lives in Kerrisdale, works as a doula, an administrator at a midwives centre and teaches yoga.
The siblings’ mother, Jackie, lives in her basement.
 Colin Ross with his sister, Bir, and parents Jackie and Colin in an undated photograph. Photo courtesy Bir Kaur O’Flaherty
Colin Ross with his sister, Bir, and parents Jackie and Colin in an undated photograph. Photo courtesy Bir Kaur O’Flaherty
Ross has had a challenging relationship with his parents, but said he is now close with his mother. His father, also named Colin, is still in his life, however tenuous the connection may be.
But it’s always been his sister he’s leaned on, which he again did a couple of weeks ago.
That trip to Alberta he was looking forward to?
He didn’t make it.
He called his sister in tears somewhere between Vancouver and the Abbotsford International Airport. He missed the last afternoon bus to the airport by eight minutes. The plane left without him, and he was unable to recoup any of the money he spent on the ticket.
“It was shitty, just really shitty and it was the first time I'd been worried about him in a long time," she said. "He turned his phone off and I didn't hear from him for two or three days."
He eventually showed up at her son's baseball game, where he took his niece to a playground. He didn't look as rough as she thought he would. He seemed content, happy to be there.
"What I came to realize probably a good eight or so years ago is that my version of OK and his version of OK are two very different things,” she said. “So for me to look at his life based on what that would feel like for me, it's very not OK. But for him, when I look at where he is now, he's doing spectacularly well, comparatively."
That's when the conversation turns to Dr. Tu, whom she described as amazing. His quality of care convinced her that Ross is in good hands. Without Tu, without the treatment options, his subsidized apartment, the advocacy work, O'Flaherty is confident her brother would be dead.
"Like a long time ago," she said.
If he were a boy in today’s world, O’Flaherty believes her brother would be on a different path. As a child, he was hypersensitive, intelligent and talented. He was bored in school.
“They know about this now, and deal with it differently,” she said
O’Flaherty continues to have hope for her brother. He is showing signs of being more present and more comfortable in his own skin.
"In some ways, he's doing better than I've ever seen him doing. The anxiety has really lessened by quite a lot, and he's able to be open and honest with my mom and me with what's happening in his life."
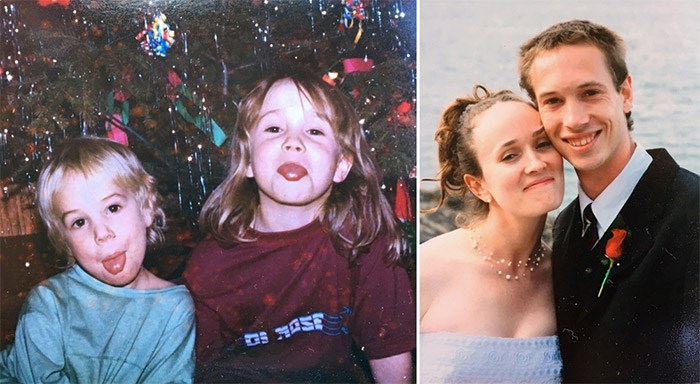 Colin Ross and his sister, Bir, as young kids and on Bir’s wedding day. Photo courtesy Bir Kaur O’Flaherty
Colin Ross and his sister, Bir, as young kids and on Bir’s wedding day. Photo courtesy Bir Kaur O’Flaherty
One day at a time
So what happens next for Colin Ross?
Last week, over coffee at a Main Street cafe, he said he hadn’t slept in three days. He was still taking the long-acting morphine, but was continuing to use heroin.
Evidence of that was his drug dealer buzzing his phone with text messages.
He talked a little bit about his failed trip to Alberta, shaking his head in disgust as he explained what happened.
“So I spent a whole bunch of money to go to Surrey for the day,” he said. “That was my vacation. It was a big, big letdown.”
He’s still waiting to hear from Megaphone Magazine about the speakers’ bureau. He’s likely to get more speaking gigs via the city’s lived experience committee when school is back in session. His doctor also talked about having him speak at his kids’ school.
He needs a purpose, he said. Idle time is not good for him.
While he’s talking about what he needs, he wants more to be done on the treatment front for drug users. Don’t get him wrong, he said, he is grateful to live in a city and province that is progressive in its drug policy.
But why isn’t there more widespread availability of medical grade heroin? Why can’t he take prescribed drugs home with him? Why does he have to be tied to a pharmacy up to three times a day?
Ross understands not every drug user can be trusted in a take-home program. But then, he said, assess each person’s situation and create a plan that works for the individual, not hinders efforts to get better.
Because right now, he said, nothing beats the high he gets from the heroin he buys in the streets, where hundreds have died.
Will he ever be abstinent?
“I was thinking about that the other day. If things I need to happen in my life happen, and I can move forward, then I do see abstinence in my future. But if I spend another couple of years in this situation, I’m starting to get dug in and I don’t know that I’ll ever get out.”
For now, it’s one day at a time.
“I’ve accepted myself for who I am, and I’m trying to make the best of it,” he said. “Maybe my life is supposed to be silver, not gold.”
@Howellings


